Two Decades Later
This backstory goes back to 2008, which wasn’t a good year for me medically. In the first five months, I had my prostate removed due to cancer. However, the cancer had metastasized beyond the prostate. A couple of months later, I had a subdural hematoma due to falling off a ladder and hitting my head against a retaining wall. I don’t recall falling or spending four weeks in the ICU at St. Mary’s Hospital.
The neurosurgeon told my family the surgery might take several hours and that I had a 50/50 chance of being alive after the surgery. The neurosurgeon had to cut a bagel-sized part of the left side of my head to relieve the high blood pressure due to the bleeding in my brain.
One of my family members took this photo of me after making it through the surgical procedure. Apparently, I was reading the latest on the stock market in the financial section of the paper. Honestly, I have no idea what I said or did during that month.
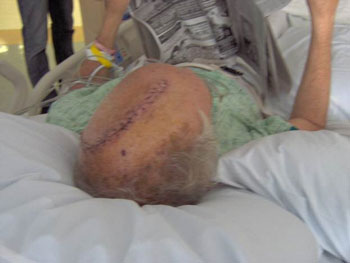
I was released from St. Mary’s and taken to a rehab hospital for another three weeks of treatment. For the first half of the time at the rehab hospital, I remained in amnesia. When I came out of my amnesia, I wanted to know where I was, why I was wearing a helmet, and why my bed was a padded playpen for an adult. I felt like the guy in this video. Nonetheless, I recovered from the metastasized prostate cancer and the subdural hematoma.
Ten years later, I took a sleep study and was told that I needed to use a CPAP when going to sleep at night. I’m on my second unit. Having said that, I’m still tired during the day and will fall asleep watching the news at noon on TV. From what I understand, there are two approaches to medically dealing with sleep apnea. I see a pulmonologist, who has increased my CPAP number from 9 to 14 and has prescribed me meds to take before I go to bed. I’ll be seeing him next week. It will be interesting to see if there are any further changes to his treatment plan.
The other medical field that treats sleep apnea is neurology. I don’t know any neurologist other than the one who did the post-operative exam at St. Mary's Hospital while I was in the ICU.

Actually, I was told by my family that Dr. Simaga examined me while I was in the ICU. Michelle said that he asked whether you knew who the people in the room were. My retort was, "I've never seen these people in my life." She said that Dr. Simaga rolled his eyes as he looked at us, because we knew you were joking. Dr. Simaga assured them that I’d be fine.
After I returned from the rehab hospital and began to get back to a normal life, I heard my flippant comment about not knowing who my family was. However, the thing that I remember the most was Dr. Simaga's comment that I would recover fully. I had spent nearly two months on my back. Returning home, I began to walk each day and gradually walked around the lake on which I live. I still walk around the lake, which takes about an hour.
When I called Dr. Simaga’s office, I knew he wasn’t taking new patients. I hoped that I could at least have him recommend a neurologist for me to see. I briefly recounted the story about his visit to check on me in the ICU. The person said that she would get back to me. The next day, I got the call and was told that I had been a patient. Therefore, my appointment is scheduled for May 12.
You can’t imagine how happy I am about the past two decades seeing Dr. Simaga. Twenty years ago, I hardly had the energy to walk a hundred feet. Today, my sleep apnea causes me to feel drained even at the beginning of the day.
My appointment with Dr. Simaga will reconnect some electrical signals to hundreds of millions of synapses in my brain. For nearly two decades, I rarely thought about the details of my dance with death due to my subdural hematoma. That dance awakened me to my clock ticking. It parallels Randy Pausch’s The Last Lecture. Seeing Dr. Simaga in a couple of weeks has awakened me to my wanting to remember the past. That duality fascinates me.

















